Your complete guide to safe exercise during pregnancy and postpartum. Learn about safety guidelines, core exercises, contraindications, and how to fuel your body for a healthy, active pregnancy.
Navigating the world of exercise during pregnancy can feel overwhelming, filled with conflicting advice. Yet, staying active is one of the most beneficial things you can do for your health and your baby’s. This guide provides a clear, evidence-based roadmap to help you exercise safely and confidently from the first trimester to your postpartum recovery.
Key Point: For most healthy pregnancies, regular physical activity is not only safe but highly recommended for managing weight gain, reducing complication risks, and improving mental well-being.
| Trimester | Frequency | Intensity (RPE 1-10) | Time | Example Activities |
|---|---|---|---|---|
| First | 3-5 days/week | 3-5 (Light to Moderate) | 30-45 min/session | Brisk walking, swimming, prenatal yoga, stationary cycling |
| Second | 3-5 days/week | 4-6 (Moderate) | 30-60 min/session | Continue first-trimester activities, add modified strength training |
| Third | 3-5 days/week | 2-4 (Light to Moderate) | 30 min/session | Focus on low-impact activities; walking, water aerobics, stretching |
The “How-To”: Safe Exercise Guidelines (Amount & Intensity)
The foundational question for most expectant mothers is, “How much is enough, and how much is too much?”. Leading health organizations, like the American College of Obstetricians and Gynecologists (ACOG), recommend at least 150 minutes of moderate-intensity aerobic activity each week. Moderate intensity means you can still hold a conversation while exercising—a technique known as the “talk test”. It is crucial to listen to your body and adjust as your pregnancy progresses, as what felt comfortable in the first trimester may need modification in the third. Always consult your healthcare provider for personalized advice.
Key Point: The “talk test” is a simple and effective way to monitor moderate intensity, ensuring you are exercising safely for both you and your baby.
Core Concerns: Strengthening the Pelvic Floor & Managing Diastasis Recti
Your core is more than just your abs; it’s a complex system that includes your pelvic floor muscles. During pregnancy, hormonal changes and the weight of your growing baby place immense pressure on these structures, potentially leading to issues like incontinence or diastasis recti (the separation of the abdominal muscles). Incorporating targeted exercises can significantly improve support and aid in postpartum recovery.
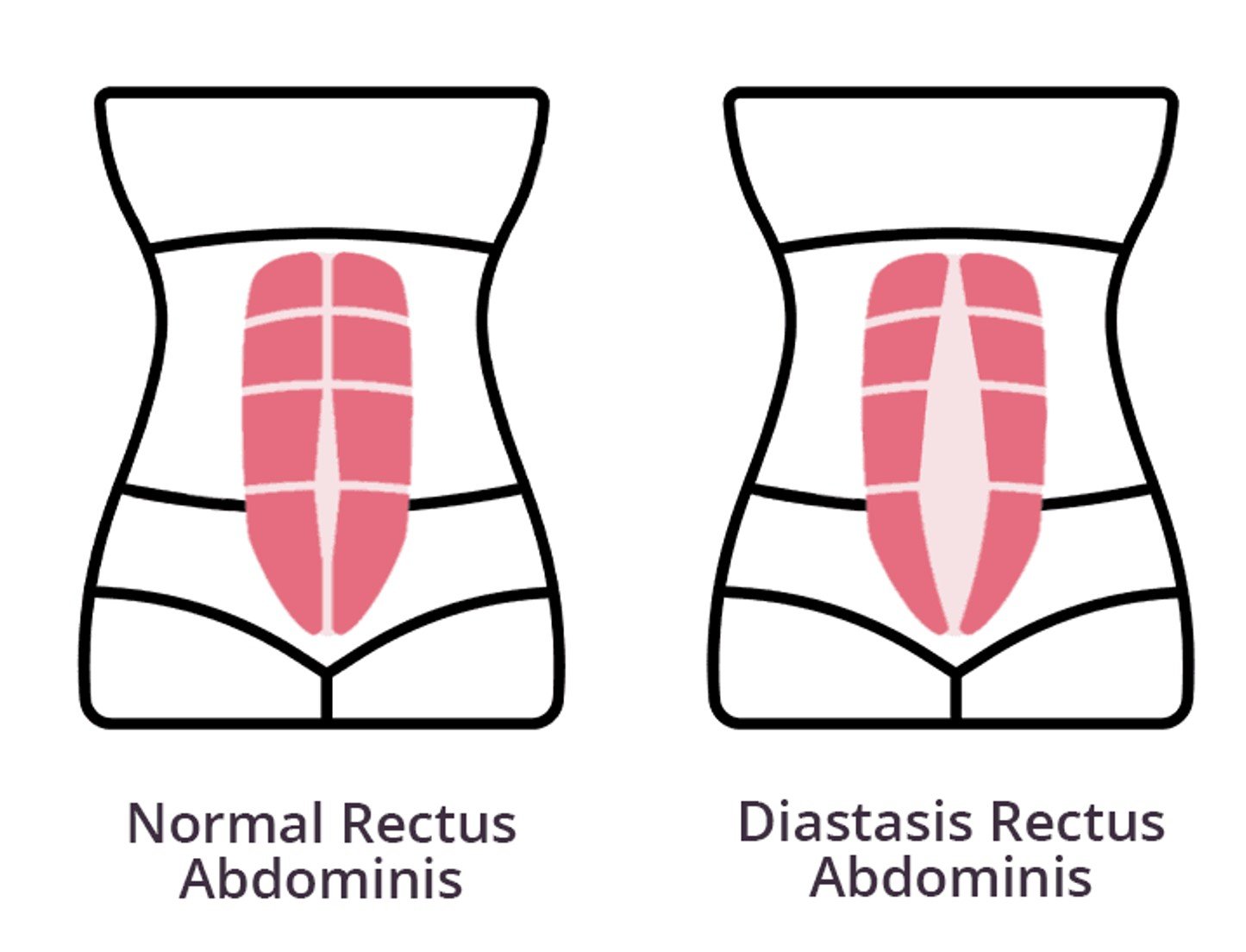
Gentle exercises like pelvic tilts, bird-dog, and diaphragmatic breathing are excellent for maintaining core stability without straining the abdominal wall. It is vital to avoid traditional crunches, sit-ups, and heavy lifting, which can worsen abdominal separation. Consulting a pelvic floor physical therapist can provide a tailored and safe exercise plan.
Key Point: Strengthening the pelvic floor with targeted exercises like pelvic tilts is crucial, while avoiding traditional crunches helps prevent worsening abdominal separation.
Fueling for Two: Hydration, Nutrition, and Thermoregulation Needs
Exercise increases your body’s demand for fuel and fluids, and this is even more true during pregnancy. Proper hydration is essential for maintaining amniotic fluid levels and supporting increased blood volume, so drink water before, during, and after your workouts. Your nutritional needs also increase, requiring an extra 300-400 calories per day in the second and third trimesters to support both your activity and your baby’s growth.

Thermoregulation, or managing your body’s internal temperature, is another key consideration. Overheating can pose risks, so avoid exercising in hot, humid conditions, opt for breathable clothing, and be mindful of your body’s signals.
Key Point: Proper hydration, an extra 300-400 calories daily in later trimesters, and avoiding overheating are essential for fueling your workouts safely.
Know the Red Flags: Safety, Contraindications, and When to Stop
While exercise is beneficial, certain medical conditions like restrictive lung disease or severe anemia are absolute contraindications, meaning exercise should be avoided unless cleared by a doctor. For all exercising mothers, it is critical to recognize warning signs that indicate you should stop immediately and contact your healthcare provider. These symptoms should never be ignored.
| Symptom / Warning Sign | Action |
|---|---|
| Vaginal bleeding or fluid leakage | Stop immediately & contact provider |
| Dizziness or feeling faint | Stop immediately & rest; contact provider if it persists |
| Chest pain or severe headache | Stop immediately & seek medical attention |
| Regular, painful contractions | Stop immediately & contact provider |
| Calf pain or swelling | Stop immediately & contact provider (risk of blood clot) |
Key Point: Always prioritize safety by recognizing warning signs like vaginal bleeding, dizziness, or chest pain, and stop exercising immediately to contact your provider if they occur.
The Fourth Trimester: A Guide to Postpartum Recovery and Return-to-Play

The journey doesn’t end at delivery. The postpartum period is a critical time for healing, and rushing back into high-intensity exercise can cause injury. The focus should initially be on rest and gentle functional movements. A gradual return-to-play strategy is safest, beginning with walking and pelvic floor exercises once cleared by your provider (typically around 6 weeks postpartum). From there, you can slowly reintroduce more intensity, always listening to your body.
Key Point: Postpartum recovery requires a gradual return to exercise, starting with gentle movements like walking after receiving clearance from your healthcare provider.
Takeaway
Staying active during pregnancy is a powerful act of self-care with profound benefits for both mother and child. By focusing on safety, listening to your body, and communicating with your healthcare provider, you can build a routine that supports a healthy, strong, and empowered pregnancy journey.
“Regular physical activity during pregnancy has been shown to have minimal risks and has been proven to benefit most women.”
RESOURCE CONTENT
References
- American College of Obstetricians and Gynecologists. Physical activity and exercise during pregnancy and the postpartum period. Committee Opinion No. 804. Obstet Gynecol. 2020;135(4):e178-e188.
- Mottola MF, Davenport MH, Ruchat SM, et al. 2019 Canadian guideline for physical activity throughout pregnancy. Br J Sports Med. 2018;52(21):1339-1346.
- Benjamin DR, van de Water ATM, Peiris CL. Effects of exercise on diastasis of the rectus abdominis muscle in the antenatal and postnatal periods: a systematic review. Phys Ther. 2014;94(3):298-313.
- Bø K, Artal R, Barakat R, et al. Exercise and pregnancy in recreational and elite athletes: 2016 evidence summary from the IOC expert group meeting, Lausanne. Part 1—exercise in women planning pregnancy and those who are pregnant. Br J Sports Med. 2016;50(10):571-586.
- Jorge R, Teixeira D Ferreira I, et al. Diet Recommendations for the Pregnant Exerciser and Athlete. In: Santos-Rocha R. Exercise and Physical Activity During Pregnancy and Postpartum. Springer. 2022.
Useful Resources
- Explore ACOG’s Guidelines: Visit the American College of Obstetricians and Gynecologists’ patient page on Exercise During Pregnancy for trusted, in-depth information.
- Find a Pelvic Health Physical Therapist: Use the APTA Pelvic Health Directory to find a specialized therapist in your area for personalized core and pelvic floor guidance.
FAQs
- Can I continue high-intensity training if I was an athlete before pregnancy?
Many athletes can continue a modified training regimen, but it requires close supervision from a healthcare provider. High-impact and high-risk activities should be avoided. Learn more at Team USA’s guidance for pregnant athletes. - Does exercise affect breast milk production or lactation?
No, research shows that moderate exercise does not negatively impact milk supply or composition. It is important to stay well-hydrated and consume adequate calories. Find more details at La Leche League International. - Can I start exercising during pregnancy if I was sedentary before?
Yes, you can! It is a great time to begin. Start slowly with low-impact activities like walking or swimming for 15-20 minutes a day and gradually increase as you feel comfortable. Always get medical clearance first.



Leave a Reply