Introduction
Did you know that a brisk walk can act on your muscle cells in a way remarkably similar to some of the most common diabetes medications? In the world of diabetes management, the debate of “diabetes meds vs exercise” is a common one. While both are crucial for managing type 2 diabetes, they work through different, fascinating physiological pathways.[1] This article will compare the unique mechanisms of these powerful tools, revealing what each can do, what they can’t, and how they work best together.
| Objective | You Will Understand… |
|---|---|
| Pharmacological Mechanisms | How different classes of diabetes drugs target specific organs like the liver and kidneys. |
| Lifestyle Mechanisms | How exercise and nutrition improve the body’s natural ability to use insulin and absorb glucose. |
| Synergistic Effects | Why combining medication and lifestyle changes leads to the most effective diabetes management. |
The Pharmacological Toolkit: How Diabetes Meds Work
Diabetes medications are precision tools designed to intervene at specific points in the body’s metabolism. For an undergraduate science student, it’s helpful to think of them as targeting different systems. For instance, Metformin, often the first drug prescribed, works primarily by telling the liver to produce less glucose.[2] Newer classes are even more specialized. GLP-1 receptor agonists (like Ozempic) mimic a gut hormone to tell the pancreas to release more insulin after a meal. Meanwhile, SGLT2 inhibitors have a completely different strategy: they work on the kidneys, causing excess glucose to be flushed out of the body through urine.[3]
Key Point: Meds offer highly specific biochemical interventions, like forcing glucose out through urine or blocking its production, actions which lifestyle changes alone cannot replicate.
The Body’s Own Medicine: Exercise & Nutrition
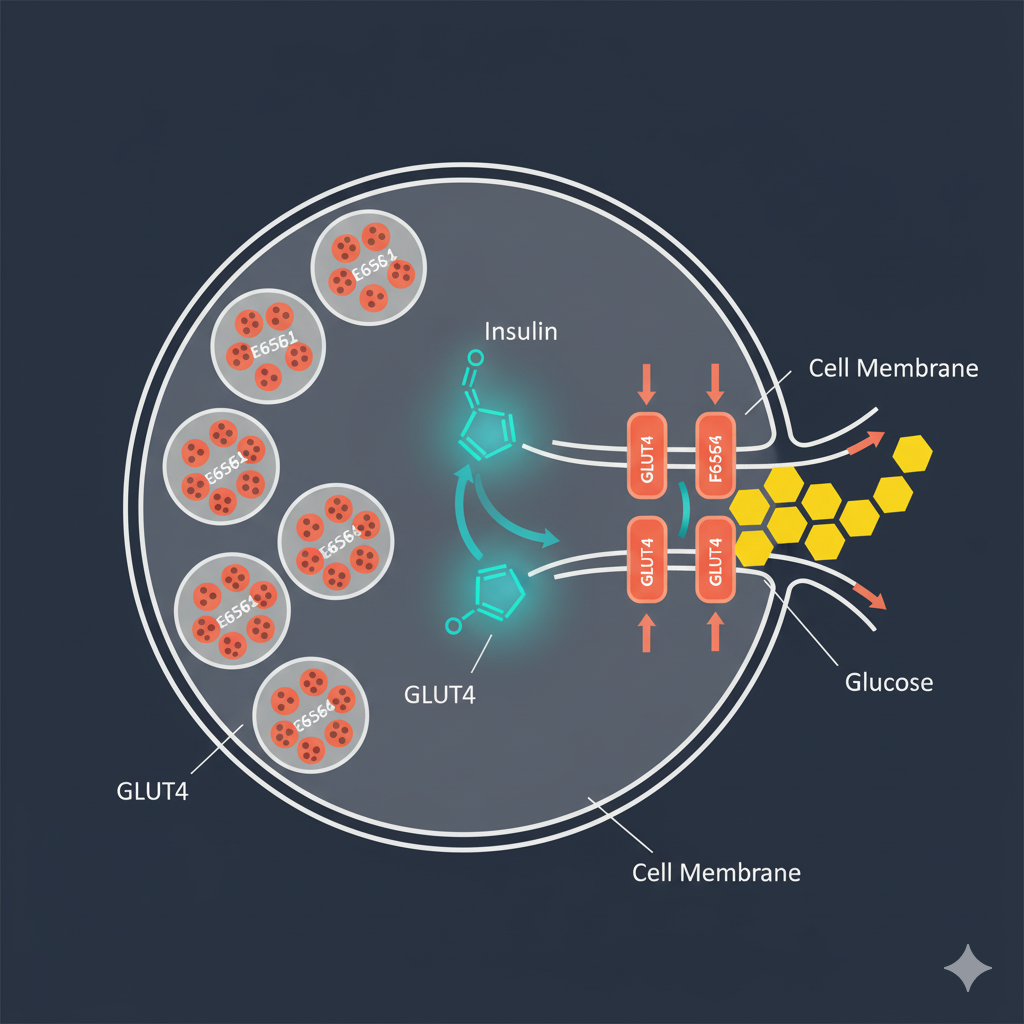
If medications are the precision tools, lifestyle changes are the master key to improving your body’s entire metabolic engine. When you exercise, your skeletal muscles—the biggest consumers of glucose in your body—can pull sugar from the blood without needing much insulin at all. This happens because muscle contractions trigger special glucose doorways, called GLUT4 transporters, to move to the cell surface and let glucose in.[4] It’s a powerful, natural mechanism for lowering blood sugar. Similarly, a balanced diet rich in fiber and complex carbohydrates improves your body’s overall sensitivity to insulin, meaning the insulin you do produce works much more efficiently.
| Exercise Type | Primary Benefit for Glycemic Control |
|---|---|
| Aerobic Exercise (e.g., running, cycling) | Improves insulin sensitivity and cardiovascular health, using glucose for sustained energy.[5] |
| Resistance Exercise (e.g., weightlifting) | Builds muscle mass, which acts as a larger “storage tank” for glucose, improving long-term blood sugar stability.[6] |
Key Point: Lifestyle interventions provide broad metabolic benefits and improve how the body’s own systems function, a holistic effect that a single pill can’t achieve.
Synergy: Integrating Meds and Lifestyle for Optimal Control
So which is better? The answer is neither. The most effective diabetes management comes from synergy. Think of it this way: if metformin is turning down the glucose “faucet” from the liver, exercise is opening up the “drain” in the muscles. Using both at the same time is far more effective than either one alone.[7] This integrated approach often means a person can achieve their blood sugar goals with a lower dose of medication. Furthermore, while medications are excellent at controlling glucose, they don’t typically offer the vast, non-overlapping benefits of lifestyle changes, such as improved cardiovascular health, stronger bones, and better mental well-being.[8]
Key Point: The goal isn’t to choose one over the other, but to use them synergistically for comprehensive diabetes management.
Takeaway
Ultimately, understanding the “diabetes meds vs exercise” debate reveals that they are powerful partners, not rivals. Medications provide targeted, potent control over biochemical pathways, while exercise and nutrition improve the body’s fundamental metabolic health in a way no pill can.
“Medication provides the precision, but lifestyle provides the foundation. True diabetes control is built on both.”
References
- American Diabetes Association Professional Practice Committee. Standards of Care in Diabetes-2024. Diabetes Care. 2024;47(Supplement 1):S1-S321. doi:10.2337/dc24-SINT.
- Hostalek U. Global epidemiology of metformin intolerance. Diabet Med. 2019;36(8):949-962. doi:10.1111/dme.13848.
- Zelniker TA, Braunwald E. Mechanisms of Cardiorenal Effects of SGLT2 Inhibitors: JACC State-of-the-Art Review. J Am Coll Cardiol. 2020;75(4):422-434. doi:10.1016/j.jacc.2019.11.031.
- Richter EA, Hargreaves M. Exercise, GLUT4, and skeletal muscle glucose uptake. Physiol Rev. 2013;93(3):993-1017. doi:10.1152/physrev.00038.2012. PMID: 23899560
- Colberg SR, Sigal RJ, Yardley JE, et al. Physical Activity/Exercise and Diabetes: A Position Statement of the American Diabetes Association. Diabetes Care. 2016;39(11):2065-2079. doi:10.2337/dc16-1728. >
- Lee J, Kim D, Kim C. The Effects of Resistance Training in People With Type 2 Diabetes Mellitus: A Systematic Review and Meta-Analysis. J Clin Med. 2019;8(9):1315. doi:10.3390/jcm8091315. PMID: 31480353
- Boulé NG, Haddad E, Kenny GP, Wells GA, Sigal RJ. Effects of exercise on glycemic control and body mass in type 2 diabetes mellitus: a meta-analysis. JAMA. 2001;286(10):1218-27. doi:10.1001/jama.286.10.1218. PMID: 11559268
- Warburton DE, Nicol CW, Bredin SS. Health benefits of physical activity: the evidence. CMAJ. 2006;174(6):801-9. doi:10.1503/cmaj.051418.
Useful Resources
- American Diabetes Association (ADA): The leading authority on diabetes care, research, and advocacy.
- CDC – Managing Diabetes: Provides practical tips and information for living with diabetes.
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK): Offers in-depth scientific information on diabetes research.
- American College of Sports Medicine (ACSM): Provides evidence-based guidelines on exercise for various health conditions, including diabetes.
Frequently Asked Questions
Can I stop my meds if I exercise enough?
Never stop or change your medication without consulting your doctor. While exercise can significantly improve blood sugar control and may lead to a reduction in medication dosage, it is rarely a complete substitute, especially in long-standing diabetes. You can read more in the ADA’s fitness guidelines.
What’s the best type of exercise for blood sugar?
The most effective approach is a combination of aerobic and resistance exercise. As the ACSM recommends, aiming for at least 150 minutes of moderate-intensity aerobic activity and two sessions of resistance training per week is ideal.
Do I need to change my diet if I’m on medication?
Yes. Medication is a tool to help manage blood sugar, but it does not replace the need for a healthy diet. Medical nutrition therapy is a cornerstone of all diabetes management plans, as detailed by the NIDDK.
How long does it take for exercise to lower blood sugar?
The blood sugar-lowering effects of a single bout of exercise can last for 24 to 48 hours. This is why regular, consistent physical activity is so important. Learn more about the immediate effects from the CDC.
Are newer drugs like Ozempic a substitute for lifestyle changes?
No. While GLP-1 agonists are very effective for both blood sugar control and weight loss, they are most effective when used as part of a comprehensive plan that includes diet and exercise. All major clinical trials for these drugs, like the SUSTAIN-6 trial, involved patients who were also advised on lifestyle modification.
Future Blog Topics
| Upcoming Article | Coming Soon | Why It Matters |
|---|---|---|
| The Gut Microbiome and Diabetes | November 2025 | Discover how the bacteria in your gut can influence blood sugar and insulin resistance. |
| Wearable Tech for Glucose Monitoring | December 2025 | A look at the science behind continuous glucose monitors (CGMs) and future non-invasive tech. |
| The Genetics of Type 2 Diabetes | January 2026 | Explore the genes that can increase your risk and what they mean for prevention and treatment. |


Leave a Reply