Most people with type 2 diabetes don’t realize that their morning jog activates the same cellular machinery that their metformin prescription targets.[1] This convergence isn’t coincidental—it reveals a fundamental truth about how our bodies regulate blood glucose control at the molecular level.
Over 37 million Americans live with diabetes, and the vast majority struggle with insulin resistance rather than insulin deficiency.[2] Understanding GLUT4—the glucose transporter protein that serves as the gateway for glucose entry into muscle and fat cells—transforms how we approach diabetes management. Furthermore, this knowledge empowers patients to see themselves not as passive medication recipients but as active participants in their cellular health.
Key Point: Insulin sensitizers, aerobic exercise, and dietary choices all converge on a common pathway: optimizing GLUT4-mediated glucose metabolism in muscle and fat cells.[3]
What You’ll Learn
| Learning Objective | What You’ll Gain |
|---|---|
| Understand how GLUT4 regulates glucose uptake | Knowledge of the cellular mechanism underlying blood sugar control |
| Learn how medications activate GLUT4 | Insight into why insulin sensitizers work at the molecular level |
| Discover exercise’s role in GLUT4 activation | Practical strategies to enhance insulin sensitivity without drugs |
| Explore nutrition’s impact on glucose metabolism | Evidence-based dietary approaches to optimize GLUT4 function |
How Insulin Sensitizers Work: The GLUT4 Connection
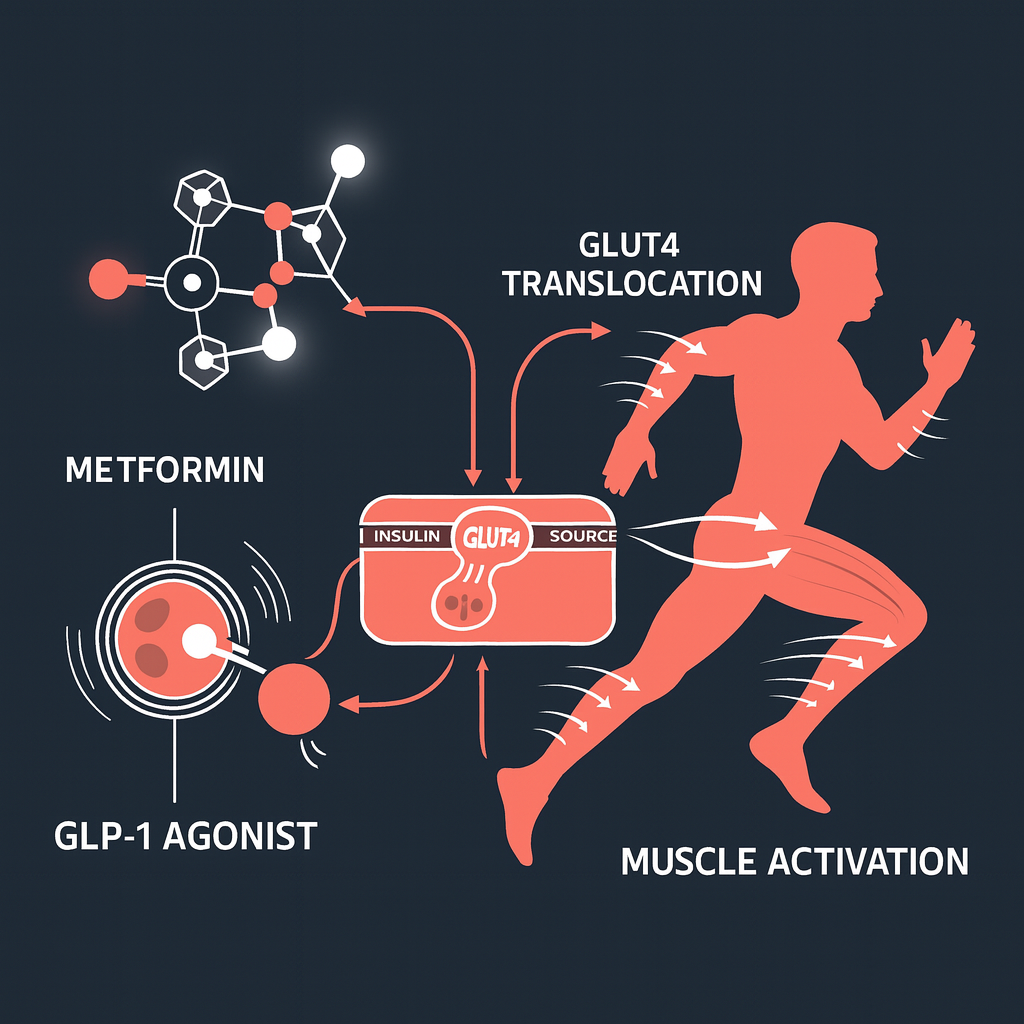
Insulin sensitizers like metformin represent the cornerstone of type 2 diabetes medication management, yet their mechanism centers on enhancing a process your body already performs naturally.[4] These medications don’t force glucose into cells; instead, they amplify the cellular response to insulin, primarily by promoting GLUT4 translocation to the cell membrane. Consequently, muscle and adipose tissue become more receptive to insulin’s signal, allowing glucose to enter cells more efficiently.
The medication types available target different aspects of this pathway. Metformin activates AMPK (AMP-activated protein kinase), an energy sensor that triggers GLUT4 movement even in insulin-resistant states.[5] Thiazolidinediones work through different nuclear receptors but ultimately achieve the same goal: more GLUT4 at the membrane means better glucose uptake.[6] Moreover, newer medications like GLP-1 agonists enhance this system by improving pancreatic beta cell function while also supporting GLUT4-mediated glucose disposal.
Key Point: Medications don’t create new biology—they enhance existing cellular pathways that regulate how your muscles and fat tissue absorb glucose.
Exercise as Medicine: Activating GLUT4 Without Drugs
Here’s where the story becomes truly empowering: aerobic exercise activates the same GLUT4 translocation pathway that medications target, but through a completely different molecular switch.[7] When you exercise, muscle contractions trigger AMPK activation independent of insulin, commanding GLUT4 vesicles to move to the membrane. Therefore, physical activity provides insulin-independent glucose uptake—a critical advantage for people with insulin resistance.
The effects are both immediate and long-lasting. A single bout of moderate aerobic exercise increases glucose uptake for up to 48 hours afterward as GLUT4 remains elevated at the cell surface.[8] Additionally, regular training increases total GLUT4 protein expression, meaning your muscles produce more transporters overall—essentially upgrading your cellular glucose disposal capacity.
| Exercise Type | Intensity | Duration | GLUT4 Effect |
|---|---|---|---|
| Brisk Walking | Moderate (50-70% max HR) | 30-45 minutes | Increased translocation for 24-48 hours |
| Jogging/Running | Vigorous (70-85% max HR) | 20-30 minutes | Enhanced AMPK activation, prolonged glucose uptake |
| Resistance Training | Moderate-High (60-80% 1RM) | 45-60 minutes | Increased GLUT4 protein expression, muscle mass gains |
| HIIT (Intervals) | High (85-95% max HR) | 15-20 minutes | Maximal AMPK response, efficient time investment |
Key Point: Every workout is a dose of cellular medicine—no prescription required. Exercise provides insulin-independent glucose uptake through AMPK activation.
Nutrition’s Role: Fueling the GLUT4 System
While exercise and medication activate GLUT4, nutrition determines what flows through these transporters and how efficiently the system operates.[9] Strategic carbohydrate timing—consuming complex carbs before exercise and faster-digesting carbs immediately after—capitalizes on exercise-induced GLUT4 translocation. During this “metabolic window,” glucose uptake occurs with minimal insulin requirement, effectively bypassing insulin resistance.
Beyond timing, macronutrient quality matters significantly for GLUT4 function. Omega-3 fatty acids improve cell membrane fluidity, facilitating GLUT4 insertion into the membrane.[10] Adequate protein intake supports muscle mass maintenance, which is critical since muscle tissue contains the highest concentration of GLUT4 transporters. Furthermore, specific micronutrients like magnesium and vitamin D play essential roles in insulin signaling pathways that regulate GLUT4 activity.
Key Point: Strategic nutrition amplifies both medication and exercise benefits by optimizing the substrate and cellular environment for GLUT4-mediated glucose metabolism.
Taking Control: The Convergence Strategy
The convergence of medication, exercise, and nutrition on the GLUT4 pathway reveals a profound truth: diabetes management isn’t about choosing between pharmaceutical and lifestyle interventions—it’s about leveraging their synergistic effects. Each approach activates GLUT4 through different mechanisms, creating multiple pathways to the same beneficial outcome. Therefore, patients who combine insulin sensitizers with regular aerobic exercise and strategic nutrition aren’t just following best practices—they’re maximizing cellular glucose disposal capacity through complementary molecular mechanisms.
“Understanding that exercise activates the same glucose transport system as medications fundamentally changes the patient’s relationship with lifestyle interventions—from optional to essential.”
— Diabetes Care Journal, 2024
References
- Richter EA, Hargreaves M. Exercise, GLUT4, and skeletal muscle glucose uptake. Physiol Rev. 2013;93(3):993-1017. doi:10.1152/physrev.00038.2012 PMID: 23899560
- Centers for Disease Control and Prevention. National Diabetes Statistics Report, 2023. Atlanta, GA: Centers for Disease Control and Prevention, U.S. Dept of Health and Human Services; 2023.
- Goodyear LJ, Kahn BB. Exercise, glucose transport, and insulin sensitivity. Annu Rev Med. 1998;49:235-261. doi:10.1146/annurev.med.49.1.235 PMID: 9509261
- Foretz M, Guigas B, Viollet B. Understanding the glucoregulatory mechanisms of metformin in type 2 diabetes mellitus. Nat Rev Endocrinol. 2019;15(10):569-589. doi:10.1038/s41574-019-0242-2 PMID: 31439934
- Viollet B, Guigas B, Sanz Garcia N, Leclerc J, Foretz M, Andreelli F. Cellular and molecular mechanisms of metformin: an overview. Clin Sci (Lond). 2012;122(6):253-270. doi:10.1042/CS20110386 PMID: 22117616
- Ahmadian M, Suh JM, Hah N, et al. PPARγ signaling and metabolism: the good, the bad and the future. Nat Med. 2013;19(5):557-566. doi:10.1038/nm.3159 PMID: 23652116
- Stanford KI, Goodyear LJ. Exercise and type 2 diabetes: molecular mechanisms regulating glucose uptake in skeletal muscle. Adv Physiol Educ. 2014;38(4):308-314. doi:10.1152/advan.00080.2014 PMID: 25434013
- Cartee GD, Wojtaszewski JF, Kunth-Velten WN. Molecular mechanisms for greater effect of post-exercise insulin on glucose uptake. Appl Physiol Nutr Metab. 2007;32(4):557-566. doi:10.1139/H07-071 PMID: 17622268
- Ivy JL, Kuo CH. Regulation of GLUT4 protein and glycogen synthase during muscle glycogen synthesis after exercise. Acta Physiol Scand. 1998;162(3):295-304. doi:10.1046/j.1365-201X.1998.0302e.x PMID: 9578375
- Salmerón J, Manson JE, Stampfer MJ, Colditz GA, Wing AL, Willett WC. Dietary fiber, glycemic load, and risk of non-insulin-dependent diabetes mellitus in women. JAMA. 1997;277(6):472-477. doi:10.1001/jama.1997.03540300040031 PMID: 9020271
Useful Resources
- American Diabetes Association – Physical Activity Guidelines: Evidence-based recommendations for exercise in diabetes management, including intensity, duration, and safety considerations.
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK): Comprehensive nutrition and physical activity resources for people with diabetes, including meal planning tools and exercise strategies.
- CDC – Get Active for Diabetes: Practical guidance on incorporating physical activity into diabetes management, with tips for getting started safely.
- Diabetes Care Journal: Leading peer-reviewed journal publishing cutting-edge research on GLUT4, exercise physiology, and diabetes interventions.
Frequently Asked Questions
How long does exercise keep GLUT4 activated at the cell membrane?
A single bout of moderate aerobic exercise increases GLUT4-mediated glucose uptake for 24-48 hours after the workout ends. This phenomenon, called “exercise-induced insulin sensitivity,” means your muscles continue absorbing glucose more efficiently even at rest. For detailed guidelines on exercise duration and intensity, see the American Diabetes Association’s exercise safety guide.
Can I reduce my diabetes medication if I exercise regularly?
Never adjust medication without consulting your healthcare provider. However, many people with type 2 diabetes who adopt consistent exercise programs do experience improved glycemic control, which may lead their doctor to reduce medication dosages over time. Regular monitoring of blood glucose and HbA1c levels is essential. Work with your endocrinologist to develop a personalized plan—find a specialist through the Endocrine Society’s physician directory.
What type of exercise is best for increasing GLUT4 and insulin sensitivity?
Both aerobic exercise and resistance training effectively activate GLUT4, but through slightly different mechanisms. Aerobic activities like brisk walking, jogging, or cycling provide immediate GLUT4 translocation and improved glucose uptake during and after exercise. Resistance training builds muscle mass, which increases your total GLUT4 capacity since muscle tissue contains the highest concentration of these transporters. The optimal approach combines both—aim for 150 minutes of moderate aerobic activity plus 2-3 resistance training sessions weekly, as recommended by the CDC diabetes management guidelines.
Does the timing of meals relative to exercise really matter for GLUT4 function?
Yes, strategic nutrient timing can significantly enhance GLUT4-mediated glucose uptake. The 30-60 minute window after exercise represents peak GLUT4 activity at the cell membrane, meaning glucose enters muscle cells with minimal insulin requirement. Consuming a combination of carbohydrates and protein during this window optimizes glycogen restoration and supports muscle recovery. For evidence-based meal timing strategies, consult the NIDDK nutrition guidelines for diabetes and consider working with a registered dietitian specializing in diabetes care.
How quickly will I see improvements in my HbA1c from lifestyle interventions?
HbA1c reflects your average blood glucose over the past 2-3 months, so significant changes typically appear within 8-12 weeks of consistent lifestyle interventions. However, daily blood glucose improvements from enhanced GLUT4 function can be observed much sooner—often within 1-2 weeks of regular exercise and dietary modifications. Track your fasting glucose and post-meal readings to see more immediate feedback on how exercise and nutrition affect your glycemic control. The American Diabetes Association’s technology resources provide guidance on effective glucose monitoring strategies.
Future Blog Topics
| Upcoming Article | Coming Soon | Why It Matters |
|---|---|---|
| Pancreatic Beta Cell Regeneration: New Hope for Type 2 Diabetes | Next Week | Discover emerging research on restoring insulin production through beta cell regeneration and protection strategies |
| Beyond Metformin: Emerging Insulin Sensitizers and SGLT2 Inhibitors | 2 Weeks | Explore new medication classes that work through novel mechanisms to improve glucose control and cardiovascular health |
| The Gut Microbiome’s Role in Glucose Metabolism and Insulin Resistance | 3 Weeks | Learn how gut bacteria influence blood sugar control and practical strategies to optimize your microbiome for better metabolic health |


Leave a Reply